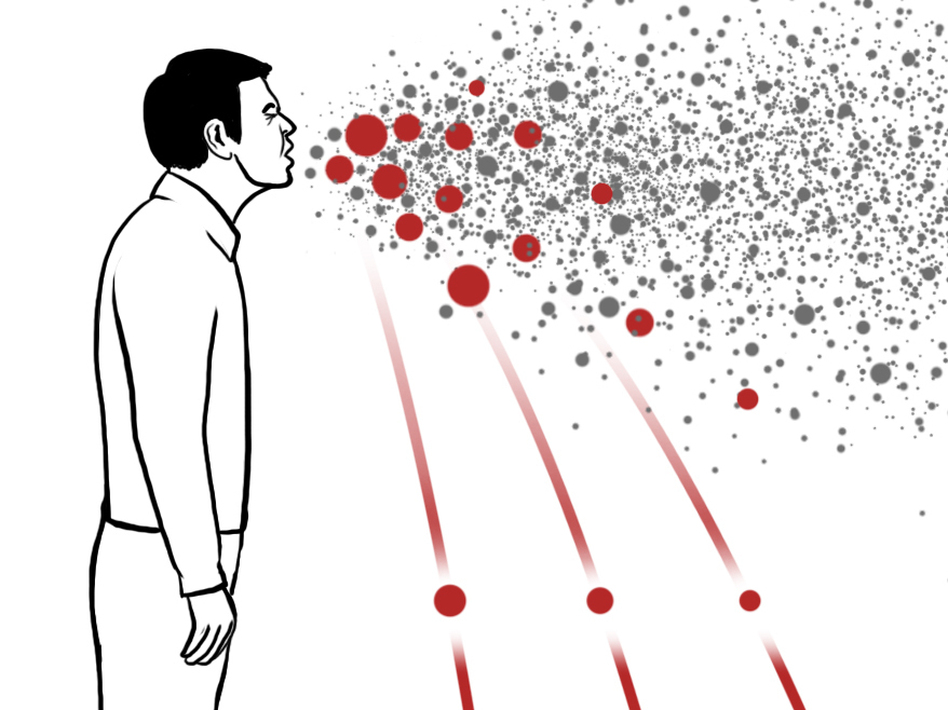
This is a strange experience, what online philosophers call cognitive dissonance. Rishi Sunak and the… Read More… Continue reading Smoking and Vaping- the beginning of the end?
Abortion rights under threat.
Reproductive health is critically important. Allowing women choice over when and with whom to have… Read More… Continue reading Abortion rights under threat.
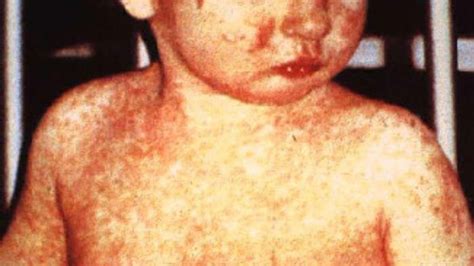
The world leading antivaxxer?
The various preventable outbreaks of measles around the world represents another step backwards for humanity.… Read More… Continue reading The world leading antivaxxer?
217 vaccines in one person!! What happened next?
This is interesting – one decidedly odd 62 year old gentleman in Germany bought and… Read More… Continue reading 217 vaccines in one person!! What happened next?
THE REAL SCANDAL OF IVERMECTIN
Ivermectin for the treatment of COVID19 has generated a huge number of conspiracy theories, much… Read More… Continue reading THE REAL SCANDAL OF IVERMECTIN
Misinformation and Trust
The doctor patient relationship can seem an abstract concept until you actually enter into one.… Read More… Continue reading Misinformation and Trust
Whole body MRI as a present? No thanks!
Well it now seems that if you want to give that VERY special present to… Read More… Continue reading Whole body MRI as a present? No thanks!
The beauty of Gene therapy
Many decades ago, as a mature A level student with lofty ambitions to become a… Read More… Continue reading The beauty of Gene therapy
Gaza 3 – The End Game
My lovely grandson recently visited my place and was scared out of his wits when… Read More… Continue reading Gaza 3 – The End Game
Gaza 2/3. NOW. Will 500,000 Palestinians die?
David vs Goliath Over the last century a pattern has emerged of Palestinian-Israeli conflict which… Read More… Continue reading Gaza 2/3. NOW. Will 500,000 Palestinians die?
Gaza 1/3 – Can understanding history help?
Well there it is. I have had a sort of writers block. Not because there… Read More… Continue reading Gaza 1/3 – Can understanding history help?
Vaccine harm and the Hippocratic oath
One thing I have noticed from those critical of modern medicine is their misuse of… Read More… Continue reading Vaccine harm and the Hippocratic oath
Misinformation 14 – Belief in BulIshit
It seems ‘Bullshit’ has been elevated to a technical term, recognised by psychologists and increasingly… Read More… Continue reading Misinformation 14 – Belief in BulIshit
Misinformation 13 – AIDS Denialism
I listened with awe to a recent documentary about the dual assassinations of Martin Luther… Read More… Continue reading Misinformation 13 – AIDS Denialism
Blood letting
Blood tests are an important part of screening, diagnosing and monitoring disease. Despite being freely… Read More… Continue reading Blood letting
Zeroes – health care staff with long COVID
How not to treat heroes It takes a leap of imagination to put yourself in… Read More… Continue reading Zeroes – health care staff with long COVID
COVID UPDATE SEPT 23
The booster programme for winter illnesses is now under way in the UK. So is… Read More… Continue reading COVID UPDATE SEPT 23
Misinformation 12 – vaccine batch quality
The latest virus to infect the internet claims huge differences in safety between batches of… Read More… Continue reading Misinformation 12 – vaccine batch quality
Unhappy 75th Birthday NHS?
It’s 75 years ago since healthcare was transformed in this country. In a war weary… Read More… Continue reading Unhappy 75th Birthday NHS?
Is RFK Jr. fit for office?
Given that many Americans see Joe Biden as too old and Trump, well, as Trump,… Read More… Continue reading Is RFK Jr. fit for office?
Vaccination, MS and misinformation.
Misinformation continues to infect the internet. Recently, a retired nurse and prolific YouTuber Dr John… Read More… Continue reading Vaccination, MS and misinformation.
The COVID Inquiry
As a species we are pretty terrible at ‘learning our lessons and moving on’, the… Read More… Continue reading The COVID Inquiry
Misinformation matters – in defence of experts
As the pandemic fades it leaves much in its wake. For some symptoms of long… Read More… Continue reading Misinformation matters – in defence of experts
Killer Conservatives
After 13 years of British Conservatism it’s time to vote again. Admittedly they are for… Read More… Continue reading Killer Conservatives
Can the wellness industry damage health?
Im a big fan of people staying as healthy as possible; staying well is decidedly… Read More… Continue reading Can the wellness industry damage health?
H5N1 – strictly for the birds?
So influenza viruses are our companion, our cohabitees in the modern world of dense human,… Read More… Continue reading H5N1 – strictly for the birds?
Is financing vaccines ethically possible?
A few years ago, I attended a review of a local planning application by a… Read More… Continue reading Is financing vaccines ethically possible?
Does vaccination increase your risk of COVID19?
Having had my second mRNA booster with the bivalent vaccine, I noted that another virus… Read More… Continue reading Does vaccination increase your risk of COVID19?
The Lab Leak or Spillover “debate”? Can we do better…
As a blogger of all things COVID over the last three years it would seem… Read More… Continue reading The Lab Leak or Spillover “debate”? Can we do better…
Vitamin D and COVID 19- hope or hype?
Introduction In a word, hype. It would be so nice to have a simple and… Read More… Continue reading Vitamin D and COVID 19- hope or hype?
Is this the worst COVID research ever?
Well, its the worst “research” I’ve come across! So bad, it’s interesting – partly because… Read More… Continue reading Is this the worst COVID research ever?
Science shortie: Do viruses really exist?
As the pandemic runs its course with its pretty awful consequences currently hitting China the… Read More… Continue reading Science shortie: Do viruses really exist?
Happy New Year – 10 reasons to be cheerful
A look at why life can be so wonderful! Happy New Year!!
Misinformation 11 – fun fighting back
Im glad to say that I’m far from alone when it comes to a sense… Read More… Continue reading Misinformation 11 – fun fighting back
COVID – winter of discontent?
It’s a strange winter already. I have a pear tree that has flowered in late… Read More… Continue reading COVID – winter of discontent?
Misinformation and the Woozle.
It seems dealing with misinformation and its deadly effects is becoming a part of doctors… Read More… Continue reading Misinformation and the Woozle.
COVID19 – why it still matters
Summary Omicron is a less severe infection for most people but will continue to cause… Read More… Continue reading COVID19 – why it still matters
COVID19 update
Hello again! I’ve not updated on COVID much recently; there are other looming realities which… Read More… Continue reading COVID19 update
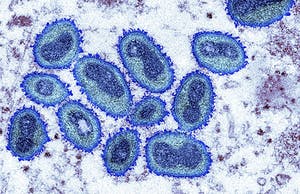
Monkeypox
To add to the many problems we face due to our destruction of the natural… Read More… Continue reading Monkeypox
Science vs social media – the Ivermectin saga.
A Star is Born What we want when it comes to illness, and desperately so… Read More… Continue reading Science vs social media – the Ivermectin saga.
The Nuclear Issue
European war is the next huge threat to global human health, shoving COVID19 and the… Read More… Continue reading The Nuclear Issue
Vitamin D and COVID19 – time to eat my hat?
It doesn’t seem to prevent COVID19. Since starting this blog, Ive written a number of… Read More… Continue reading Vitamin D and COVID19 – time to eat my hat?
Evil
Evil begets evil Just when we are in the middle of one evil, another emerges.… Read More… Continue reading Evil
April Fools?
For me, the best April fool prank was the spaghetti tree harvest from the BBC… Read More… Continue reading April Fools?
Our Great Chicken Pox Party
All of a sudden coronavirus is everywhere again. According to the ONS, 1 in 16… Read More… Continue reading Our Great Chicken Pox Party
Out of the pandemic, into the fire.
Keeping tabs on the pandemic, its science, evolution, treatment and prevention, though a sombre business,… Read More… Continue reading Out of the pandemic, into the fire.
War and pestilence – some suggestions
Sadly, everything has been turned upside down in our world. We now have a global… Read More… Continue reading War and pestilence – some suggestions
First pestilence, now war.
Just as we thought we were creeping towards the end of one major society changing… Read More… Continue reading First pestilence, now war.
The end game?
I’ve been distracted by the storm blowing over a formerly glorious oak, taking down with… Read More… Continue reading The end game?
Mandates and truckers
In a world of converging and urgent crises, the pandemic, water and food shortages, climate… Read More… Continue reading Mandates and truckers
Misinformation 10 – the “Midazolam murders”
I try to keep the blog positive, but find myself continually heading back into the… Read More… Continue reading Misinformation 10 – the “Midazolam murders”
Misinformation 9 – Another COVID death hoax.
As this phase of the pandemic evolves, many of the divisions it has exposed remain… Read More… Continue reading Misinformation 9 – Another COVID death hoax.
Mandates and Midwives
This is an unusual post for me. Below is the gist of a letter I… Read More… Continue reading Mandates and Midwives
Where did Omicron come from?
As Omicron spreads around the world I asked myself the question, where did such an… Read More… Continue reading Where did Omicron come from?
Is this the beginning of the end-emic?
The New year celebrations have come and gone and its seems 2022 is going to… Read More… Continue reading Is this the beginning of the end-emic?
Happy New Year and Omicron update
Well here we are at the end of a long year of infection with all… Read More… Continue reading Happy New Year and Omicron update
Omi-Christmas cheer?
As we approach Xmas 2021, rather like last year the news is less than festive.… Read More… Continue reading Omi-Christmas cheer?
Misinformation 8 – Vaccination and miscarriage – no risk
As Omicron spreads in winter bound Europe, boosting of immunity by vaccination is being advised… Read More… Continue reading Misinformation 8 – Vaccination and miscarriage – no risk
Omicron’s mixed bag – update
To start brightly, it seems that the evidence trickling in hints at good news. This… Read More… Continue reading Omicron’s mixed bag – update
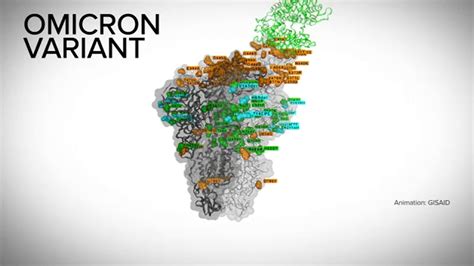
Omicron update
Omicron is very different from those variants we have seen before. There are 50 mutations,… Read More… Continue reading Omicron update
Omicron – Oh Dear!
Doesn’t it just drive you mad! Just as we are beginning to understand the dynamics… Read More… Continue reading Omicron – Oh Dear!
Misinformation 7 – Vaccination – life and death
Summary: Much anxiety has been caused by misinformation on vaccines and it seems with my… Read More… Continue reading Misinformation 7 – Vaccination – life and death
A bit of good news – new Covid treatments
With all the bad news about the pandemic across Europe, some good news is welcome.… Read More… Continue reading A bit of good news – new Covid treatments
The Human cost of Plan A
Plan A, which is essentially very little, has been playing out in the UK since… Read More… Continue reading The Human cost of Plan A
Boosters
Introduction Despite the global unmet need for vaccination the current situation means that a booster… Read More… Continue reading Boosters
Covid 19 – what will the winter bring?
This post looks at what is happening, to whom it is happening, the benefits of… Read More… Continue reading Covid 19 – what will the winter bring?
The truth about COVID transmission
Summary: The Delta wave has seen increases in COVID cases here and around the world.… Read More… Continue reading The truth about COVID transmission
Why are there so few good treatments for COVID19?
SUMMARY Antiviral treatments continue to disappoint. Monoclonals have more promise, but are expensive and tricky… Read More… Continue reading Why are there so few good treatments for COVID19?
Our new deal with the virus – is this what “Endemic” looks like?
Summary The new deal we have with the virus is now playing out. No restrictions,… Read More… Continue reading Our new deal with the virus – is this what “Endemic” looks like?
September round up
SUMMARY Release of restrictions are causing freedom for many and misery for some with 900… Read More… Continue reading September round up
Guinea pigs
SUMMARY We are now engaged in an experiment to see how vaccination, increased exposure, and… Read More… Continue reading Guinea pigs
August COVID update – our crashing wave
Summary The UK Fourth wave crashes – good news but why? The Global situation continues… Read More… Continue reading August COVID update – our crashing wave
Fourth wave chaos
Introduction. I optimistically titled my last two posts on the English summer “The light at… Read More… Continue reading Fourth wave chaos
Masking reality – masks and our kids health
Introduction Why am I writing another post on dodgy information? Haven’t I got more positive… Read More… Continue reading Masking reality – masks and our kids health
COVID19 – So is that it?
Summary Freedom day is going to be on the 19th July with just about all… Read More… Continue reading COVID19 – So is that it?
July update – light at the end of the tunnel
SUMMARY. The fourth wave looks very different from the last three with younger populations testing… Read More… Continue reading July update – light at the end of the tunnel
Misinformation 6 – Spiked information
SUMMARY A recent Channel4 documentary described the growing influence of well funded anti vaccination movement.… Read More… Continue reading Misinformation 6 – Spiked information
Fourth wave
Summary Sadly, we are now seeing a fourth SARS2 wave. Immunity from vaccination and infection… Read More… Continue reading Fourth wave
Early summer Update – clouds and silver linings
Summary To date, the vaccination programme has prevented 11,700 deaths and 33,000 hospital admissions in… Read More… Continue reading Early summer Update – clouds and silver linings
Misinformation 5 – Ivermectin’s false dawn
Summary Ivermectin is a useful drug for specified helminth (worm) infections. Claims of phenomenal cure… Read More… Continue reading Misinformation 5 – Ivermectin’s false dawn
COVID and pregnancy
A look at COVID19, pregnancy and vaccination. COVID vaccination is a pretty straightforward choice for… Read More… Continue reading COVID and pregnancy
India, the virus, and us
Summary The damaging effects of the British empire remain relevant to our relationship with India.… Read More… Continue reading India, the virus, and us
Hartlepool – are we living in a one party state?
The loss of Hartlepool is a shock for Labour. There are reasons why this happened.… Read More… Continue reading Hartlepool – are we living in a one party state?
Misinformation 4 – looking after your mind
Misinformation about the pandemic still dominates the online world. . Bad quality information can be… Read More… Continue reading Misinformation 4 – looking after your mind
April update – our crazy COVID world!
SUMMARY Optimism is in the air in the UK as cases and deaths drop, but… Read More… Continue reading April update – our crazy COVID world!
Mass screening – a real scandal
Summary We are expanding the screening of people and youngsters with no symptoms or contact… Read More… Continue reading Mass screening – a real scandal
Aztra Zenecas clotting problems
SUMMARY Problems with a rare condition affecting the smallest of cells in the blood called… Read More… Continue reading Aztra Zenecas clotting problems
Zero COVID – It is possible!
Summary Zero COVID is a philosophy which seeks to eliminate community spread of Sars-Cov2. Many… Read More… Continue reading Zero COVID – It is possible!